Anyone can get asthma, and it can start at any time of life. Asthma tends to run in families, although not everyone in the family will have it.
Asthma can be allergic or non-allergic depending on the triggers. Allergic asthma is triggered by allergens like dust mites, pollen, animal dander or mould. Non-allergic asthma can be triggered by other causes like air temperature, stress or cold and flu viruses.
Many people with allergic asthma will also have other allergic conditions like hay fever or eczema, and a family history of these conditions. A child whose parents or other close relatives already have asthma or allergies has a higher chance of developing these conditions. The chance is increased if both parents are affected.
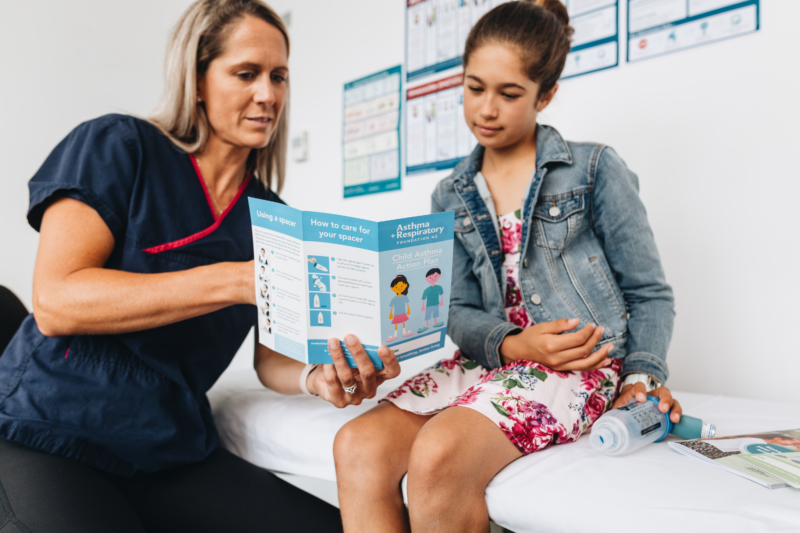
One in eight children in New Zealand experience asthma. Large numbers of children are still being admitted to hospital with asthma, and some of these will have had a potentially life-threatening asthma attack.
In children under five years of age, wheeze and coughing is common and is often triggered by a respiratory viral illness, like a cold. Not all wheezing is asthma. By school age, at least half of children who wheeze will have ‘grown out’ of their symptoms.
Although asthma cannot be cured, it can be treated. If well-managed, children can live a full and active life.
For information about asthma in children, read more.

Adult onset asthma refers to the onset of asthma for the first time in someone of middle age or older. The usual symptoms of asthma are generally present – varying degrees of breathlessness, wheeze and productive cough. However, there are some features that make adult onset asthma different to that seen in the younger age group.
Causes
We do not understand why symptoms develop at a certain age; or why they might disappear. For some people, adult onset asthma may be caused by a recurrence of childhood asthma or brought on by an illness like bronchitis.
Smoking does not cause adult onset asthma, although it can trigger an attack. Smoking is the most common cause of Chronic Obstructive Pulmonary Disease (COPD), which has similar symptoms of breathlessness, cough and sometimes wheeze. COPD is a progressive lung condition that causes narrowing of the bronchial tubes in the lungs. COPD is an ‘umbrella’ term for the diseases emphysema, chronic bronchitis and long-standing asthma. See here for more information on COPD.
One area of increasing concern is the rapid rise in the use of e-cigarettes (vaping). Many vapes contain nicotine, including products that claim to be nicotine-free. Vapes contain additives and flavours which have been approved for use in food products, but haven’t been tested as to whether they are safe when inhaled into the lungs.
While we don’t know the exact cause of asthma, we do know that asthma is believed to be caused by a combination of genetic and environmental factors. It is too early to tell how (or if) vaping plays a role in the development of asthma. However, research has so far found that vaping and second-hand vaping can irritate the lungs, cause coughing and worsen symptoms of respiratory conditions like asthma.
Sometimes other illnesses seen in adults can be hard to separate from adult onset asthma. Certain forms of heart disease which cause fluid retention can affect breathing and cause wheezing, which may seem like adult onset asthma.
Treatment
In contrast to childhood asthma, adult onset asthma is more commonly persistent and permanent. For this reason, preventative medication is prescribed to help prevent permanent damage to the lungs. Medications are often needed continuously to help keep adult onset asthma under control.
One of the difficulties in adult life is that lung function tends to fall after middle age. Certain conditions such as smoking or asthma may be associated with a faster rate of deterioration of lung function. If asthma is under-treated in adult life, there is a risk that lung function may deteriorate more quickly and never recover. In some cases it is best to use regular medication in order to protect lung function every day, rather than risk permanent deterioration. For treatment, the key issue is to maintain your best lung function at all times.

This self-management action plan for adolescents and adults (aged 12 years and over) is to be completed by healthcare practitioners, together with their patients. Available in English, te reo Māori, Samoan, Tongan and Simplified Chinese

This asthma action plan is for healthcare practitioners to complete alongside parents/caregivers and their child. Available in English, te reo Māori, Samoan and Tongan

The “Managing your child’s asthma” resource teaches parents/whānau about asthma including how to help prevent an asthma attack. Also available in English, te reo Māori, and Samoan.